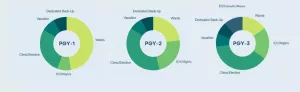
| Rotation | Length |
| General Medicine and Subspecialty Wards (Bone Marrow Transplant, Cardiology, Gastroenterology, General Medicine, Geriatrics, Heart Failure, Infectious Disease, Oncology, Pulmonary, Renal) | 22-24 weeks |
| ICU (MICU, CCU) | 4 weeks |
| Elective (Sub-specialty Clinics, Consult Services, Research, Health Disparities Elective, QI Week, Health IT Elective week) | 6-8 weeks |
| Primary Care Clinic | 8 weeks |
| Night Float (Cross Coverage Only) | 3-5 weeks |
| Dedicated Back-Up | 3-4 weeks |
| Vacation | 4 weeks |
The interns have a “2+2” structure throughout the year, where they have a two-week inpatient block, followed by a two-week block of ambulatory clinics, elective time, or back-up, known as “plus-two” blocks. For part of the year, they will have back-to-back inpatient blocks followed by a “plus-two” block (“2+2+2”), but these inpatient blocks will be in different subspecialty areas to experience new learning environments. The inpatient experiences include ward rotations at Tufts Medical Center on the Cardiology (General Cardiology/Electrophysiology and Advanced Heart Failure), Nephrology, Pulmonology, Infectious Diseases, Hematology/Oncology, General Medicine services at Tufts Medical Center (including General Medicine, Geriatrics and Gastroenterology-General Medicine) and General Medicine at Newton Wellesley Hospital.
In general, interns admit on long-call days until 7 pm approximately every fourth day during most ward rotations. There are no 24-hour shifts. Interns also get several weeks of intensive-care time in both the medical and cardiac ICUs. When rotating on night float, interns are responsible for cross-covering already admitted patients, and do not admit new patients overnight.
During “plus-two” weeks, interns are scheduled for their continuity primary care clinics and elective time, where they can request to rotate through any of our consult services or subspecialty clinics. All interns participate in a 1-week Patient Safety/Quality Improvement rotation, and they also have the chance to rotate in our health-informatics or health disparities electives. We have a dedicated back-up system, where each intern will be on backup for 3–4 weeks. During this time, they come in for morning reports and noon conferences but have no other clinical responsibilities unless called in to cover a co-intern on service or in clinic.
Intern year starts about ten days before July 1 to facilitate the house staff transition. Interns have four weeks of vacation, one of which is scheduled for the last week of intern year.