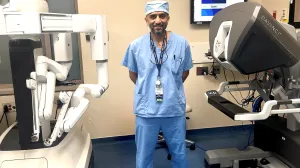
Tufts Medicine surgeons like Adam Blau, MD, Director of Robotic-Assisted Surgery at MelroseWakefield Hospital, are using robotic-assisted surgery to perform a wide array of minimally invasive procedures. Since completing our first robotic-assisted surgery in 2018, MelroseWakefield Hospital has become a regional leader, performing more than 3,500 robotic procedures in our 2 dedicated operating room suites.
Robotic-assisted surgery is now an integral part of surgical care across Tufts Medicine. Each hospital — Tufts Medical Center, Lowell General Hospital and MelroseWakefield Hospital — offers safe, technologically advanced surgical care using several robotic platforms.
“Robotic surgery is having a transformative impact at Tufts Medicine,” says Surgeon-in-Chief and Chair of Surgery Jason Hall, MD. “It’s expanding the boundaries of what is possible across a broad spectrum of surgical specialties. Our teams are leveraging robotic platforms to perform complex procedures with increased precision, improved visualization and less invasiveness — resulting in faster recoveries, shorter hospital stays and enhanced outcomes for patients.”
Robotic-assisted procedures include hernia repairs, gallbladder surgery, intestinal surgery and acid reflux surgery.
“We also treat colon cancers, diverticulitis, prostate cancer, kidney cancer, uterine and ovarian cancers and uterine fibroids with robotic surgery, as well as weight loss surgery,” says Dr. Blau. “Our surgeons even work together across different surgical specialties when needed to offer multiple operations combined into one. For example, a patient needing prostate surgery as well as a hernia repair could have both procedures performed with one operation, all through small incisions, by two collaborating surgeons.”
Surgeons are now able to use the technology for the most complex procedures, including advanced liver, gallbladder and bile duct surgeries. Teams are also expanding robotic-assisted techniques to acute care and emergency situations — helping critically ill and high-risk patients access minimally invasive procedures safely.
Extra arms, sharp eyes
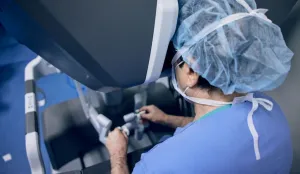
One of the robotic systems used at Tufts Medicine is the da Vinci Xi, designed for surgical precision. It features 4 robotic arms with multiple joints that handle advanced instruments, along with a high-definition 3D camera that gives surgeons exceptional depth perception. This technology allows complex operations to be performed through small incisions.
Less pain, faster recovery
This kind of precision often leads to better outcomes. Smaller incisions mean less pain after surgery, shorter hospital stays and faster returns to work and normal activities.
“With many robotic operations, patients only need to take Tylenol and Ibuprofen after surgery, without the need for narcotic pain medication. That’s not the case when the same operation is performed via a large open incision,” says Dr. Blau.
Shorter hospital stays also help reduce costs for both patients and hospitals.
Looking ahead
“We have a deep commitment to surgical innovation, interdisciplinary collaboration and excellence in both clinical care and academic training,” says Dr. Hall. “Robotic surgery is not only elevating the standard of care across our system — it is shaping the future of surgical practice.”
Learn about robotic-assisted surgery