Breast cancer forms in the breast cells, most often in the ducts carrying milk to the nipple or the glands that produce it. Breast cancer is the most common cancer among women and those assigned females at birth (AFABs), but it’s important to remember that breast cancer can affect anyone.
Your copilots in care on your breast cancer journey
An estimated 1 in 8 women and AFABs are diagnosed with breast cancer during their lifetime. Learning that you're part of that statistic can bring on a wave of emotions, so we're here to help you navigate these waters and guide you toward better health.
One of the best things you can do for your breast health is to take early action. Mammograms are the gold standard for detecting and diagnosing any suspicious breast lumps. That's why they're a staple annual exam for women and AFABs starting at age 40.
And because breast cancer can be passed down in families, you may want to learn if you have any gene mutations — like BRCA1 and BRCA2 — linked to breast cancer by pursuing genetic testing.
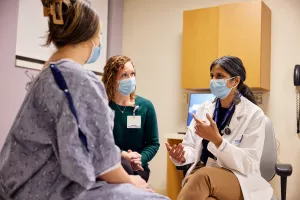
So whether you have questions about your treatment, want to join a support group or simply need someone to talk to, know that your care team will be there for you every step of the way.
Conditions
Our team provides the full suite of services for all types of breast conditions, including:
Breast cancer symptoms
Early detection is the name of the game with breast cancer. If you notice any of the following symptoms, talk to your doctor as soon as you can:
- Bleeding or crusting of the nipple
- Localized breast pain
- New breast mass
- Nipple discharge that may be clear or bloody
- Skin changes of the breast (thickening, scaling, redness, ulceration)
- Skin dimpling
- Swelling in a part of or the entire breast
- Swollen lymph nodes under the arm
Testing
Finding breast abnormalities early on helps make cancer treatments more effective. That's why we offer the full range of diagnostic options here at Tufts Medicine.
Clinical breast exams
If you are comfortable doing a breast self-exam, you can often notice early changes in your breasts that can indicate cancer. Your primary care doctor may also conduct a clinical breast exam as part of a regular check-up or if you've started experiencing breast cancer symptoms. They'll check for any changes in the size, shape, or contour of the breast by gently touching the breast and underarm area for lumps or other abnormalities.
At Tufts Medicine Breast Centers, our team of doctors, nurse practitioners, and physician assistants are skilled in checking your breasts for any changes. This is the easiest way to figure out if you need additional testing.
Breast imaging
There are several ways to take pictures (also called images) of breast tissue to look for cancers. It's a recommended and safe practice for all women and AFABs age 40 or older to schedule an annual mammogram. A mammogram is a type of X-ray that detects breast tumors and is also the gold standard for detecting early cancers in your breast. Tomosynthesis is a three-dimensional mammogram technology used in all the Tufts Medicine radiology centers that can detect very early breast cancers.
Breast ultrasound and breast MRI are other techniques used if your mammogram shows something unusual. The breast radiologists across Tufts Medicine have specialized training in all breast imaging techniques and are active partners in your clinical team.
If something unusual does show up in the breast exam or mammogram, we may recommend removing a small piece of tissue for analysis. This procedure is called a biopsy. A biopsy is usually performed by a radiologist using a needle and local anesthesia, guided by a mammogram, ultrasound, or MRI. On rare occasions, a biopsy is done by a surgeon.
Once we've confirmed that breast cancer is present in your body, it's important to understand if the cancer is spreading and, if so, how far. This process, called staging, helps us design the most effective possible care plan for you. The Tufts Medicine cancer doctors work together to determine whether staging is needed and if so, will use comprehensive staging techniques to determine whether or not your cancer has spread.
Genetic testing for breast cancer
We offer risk assessments and genetic testing to help you manage your breast health or even get one step ahead of it. Because breast cancer can be passed down through family members, we'll look for mutations in genes associated with hereditary breast cancer syndromes, such as in the BRCA1 and BRCA2 genes, to determine your risk for developing breast cancer.
We work closely with trained geneticists and genetic counselors to determine risk and perform genetic testing. If our assessment indicates an increased risk of developing breast cancer, or if testing does find one or more of these gene mutations, there are preventive methods we can explore with you, including lifestyle adjustments, medications, or surgery.
Treatments
When you’re under our care, we treat every part of you — physically, mentally and emotionally. Your care team may include the following:
- Board-certified oncologists
- Board-certified plastic surgeons
- Board-certified radiologists specializing in breast imaging
- Board-certified surgeons
- Genetic counselors
- Nurse navigators
- Physical therapists certified in lymphedema management
- Social workers
- Support groups
Together, our brightest minds in cancer care will explore whether surgery, radiation therapy, chemotherapy and other medicines or even clinical trials are the best approaches for your unique care plan.
Breast surgery is often the first step in treating breast cancer. time. Breast surgery may involve removing part of the breast (lumpectomy or partial mastectomy) or all of the breast (total mastectomy). Surgery may also include sampling the lymph nodes located under your arm. Whenever possible, we’ll use minimally invasive surgical techniques to reduce discomfort, recovery time, and complications.
There are several options for cosmetic breast reconstruction after a breast cancer treatment. Our plastic surgeons specialize in all available breast reconstruction techniques. As part of your personalized treatment plan, we will discuss with you the various options available for breast reconstruction.
We also specialize in oncoplastic breast surgery — a “2-for-1” procedure where we remove a tumor and reconstruct the breast at the same time. Only 20 or so physicians in the country perform oncoplastic breast surgery.
The good news is that based on our patient history, 90% of patients are cancer-free at the margins following oncoplastic surgery.
Radiation therapy is carefully designed by a radiation oncologist who specializes in treating patients with breast cancer. Using the latest image-guided technologies, they deliver a high-energy beam that can eliminate remaining breast cancer cells after surgery.
Radiation therapy is most often paired with surgery that preserves the breast (lumpectomy or partial mastectomy). However, sometimes it is used after surgery that removes the entire breast (mastectomy).
Our radiation oncologists work closely with your surgeon and the other members of your breast cancer team to decide whether radiation therapy should be part of your personalized treatment plan.
Medical therapy for breast cancer is carefully designed by medical oncologists who specialize in treating breast cancer. Our experts use a wide range of medications, including advanced drugs that target specific breast cancer cells.
Your care team may recommend chemotherapy, hormone therapy, precision-targeted biologic therapies, or immunotherapies before or after surgery. Our breast cancer experts work closely with the surgeons, radiation oncologists, radiologists, and pathologists on your breast cancer team to develop a personalized treatment plan specifically for you.



FAQs
The average risk for women and AFABs developing breast cancer is about 12%, or a 1 in 8 chance.
About 1 in 1,000 men and AMABs will develop breast cancer during their lifetime.
A few of the best things you can do for your breast health is:
- Stay up-to-date on your annual mammograms (once you've reached an eligible age)
- Give yourself a regular breast self-exam.
- Exercise regularly and often. A 30-minute walk every day is a great way to
lower your risk of breast cancer.
If you notice anything unusual about your breasts, contact your medical provider right away.
Like many other cancers, breast cancer risk increases as you age. Approximately 85% of cases occur in AFABs age 50 or older.
Other risk factors include:
- A genetic mutation in genes such as BRCA1 or BRCA2 or other genes such as p53 or PTEN
- A history of increased breast density on mammography
- Family history of breast or ovarian cancer
- Personal history of breast cancer (people who have had breast cancer once are at increased risk of developing it a second time)
- Prolonged estrogen exposure
- Radiation to the chest, particularly during teenage years and early adulthood
- Women and AFABs who have taken hormone replacement therapy, especially a combination of estrogen and progestagen for more than 2–3 years
- Women and AFABs who have never given birth and women who have their first child after the age of 30
- Women and AFABs who have undergone breast biopsy, primarily those with atypical hyperplasia
Women of higher socioeconomic status may be more likely to develop breast cancer. In addition, smoking appears to increase the risk of breast cancer.
The two main categories for breast cancer are non-invasive and invasive.
One type of non-invasive breast cancer is ductal carcinoma in situ (DCIS). DCIS is limited to the milk ducts, the tubes that carry milk through the breast. DCIS rarely spreads to other parts of the body. Lobular carcinoma in situ (LCIS) is usually limited to the lobules, which are the milk-producing glands inside the breast.
Invasive breast cancer refers to cancer that has spread beyond the milk ducts or lobules, which means it has the potential to spread to lymph nodes or other parts of the body. Invasive breast cancer typically comes in one of two forms: invasive ductal cancer and invasive lobular cancer.
Awards + accreditations
Our breast health and cancer care programs have been recognized for quality and safety. So when it comes to making one of the most important decisions of your life, you can be sure you’re in the best of hands.



From regular office visits to inpatient stays, find the healthcare you need and deserve close to home.
Meet the doctors and care team devoted to supporting you every step of the way along your path to better health.